Categories
Vaccination in Pregnancy: What Is Safe for Mother and Baby
Mar 08, 2026
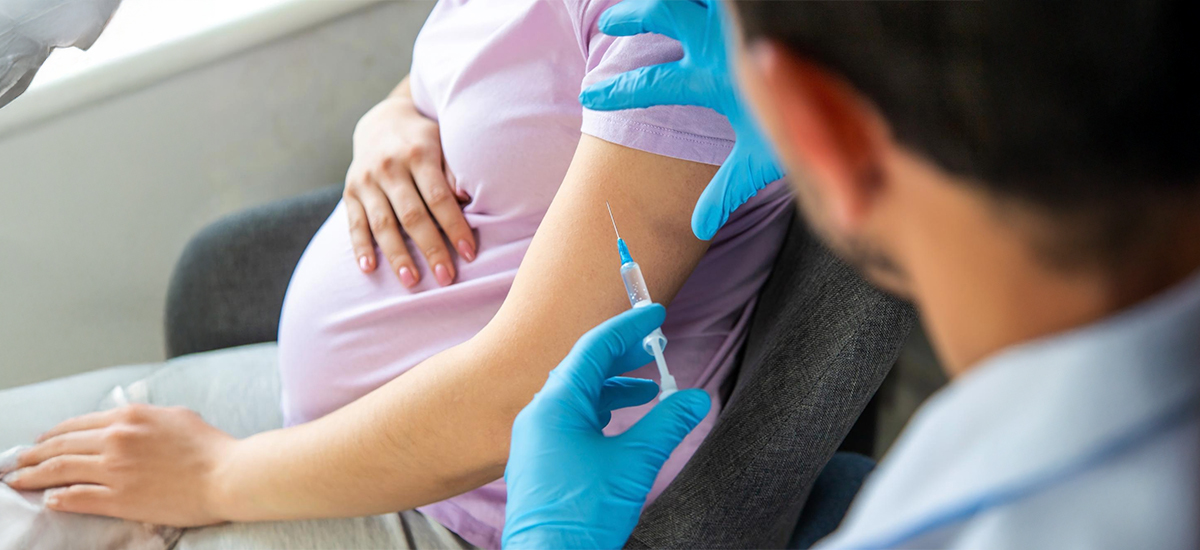
A nurse lifts a vial from a cold box, checks the label, and logs it before drawing the dose. The vial is kept cold because heat can weaken vaccines, so storage becomes part of safety. This “system thinking” entered routine care after the WHO Expanded Programme on Immunization (1974), which treated vaccines as more than injections: correct product, reliable cold chain, written records, and scheduled follow-up. Pregnancy care changed because, before this kind of organised vaccination, doctors could only react after infection struck, and newborns faced their first months without borrowed protection.
In 2026 India, the confusion is rarely about access. It is about mixed messages: an app shows “add-on vaccines”, a family WhatsApp group warns “vaccines harm the baby”, and a busy clinic visit leaves little time for explanation. So the useful goal is not to memorise a long list. It is to understand the logic: what used to happen when pregnancy vaccines did not exist, therefore what vaccination in pregnancy prevents, and how you use it safely.
Vaccination in pregnancy and why it exists
Before pregnancy vaccines became routine, two predictable problems kept repeating:- Mothers got infections during pregnancy that became harder to handle because fever, dehydration, and breathing strain carry extra risk in pregnancy, so “wait it out” often failed.
- Newborns entered life with an immune system that is still learning, but infections do not wait for the baby’s vaccine schedule, therefore the first weeks were a high-risk gap.
Maternal immunization and how the baby benefits
Before maternal immunization, a baby’s protection started late because it began only after the baby’s own vaccines and immune responses had time to build. That delay mattered, so modern care uses a simple biological shortcut. After you get vaccinated, your immune system makes protective proteins called antibodies. Many antibodies cross the placenta, especially later in pregnancy. Therefore, the baby is born with a temporary supply of antibodies, so early-life infections are less likely to become severe while the baby’s own vaccines are still underway. This is why maternal immunization is not a slogan. It is a timing strategy designed for the newborn’s vulnerable window that existed in the pre-vaccine era.Pregnancy vaccines and what they are not
A vaccine prepares the immune system before exposure, so it reduces the chance of severe disease later. That matters because, before vaccines, families relied on isolation, home remedies, and luck, but those tools could not reliably prevent infection. Pregnancy vaccines are not:- a guarantee you will never fall sick, because protection reduces risk but does not erase it,
- a substitute for medical care if you develop fever or breathing difficulty, because vaccination prevents some infections but not all,
- a random “health add-on” you take without a plan, because timing changes whether the main benefit is for the mother, the baby, or both.
Vaccination in pregnancy and the basic safety rule about vaccine types
In the past, the bigger danger was the infection itself. Today, the safety question is more precise: which type of vaccine is used during pregnancy.Inactivated vaccines are commonly used in pregnancy
Inactivated means the vaccine cannot reproduce in your body, so it cannot “spread” as an infection. Therefore, inactivated vaccines form the backbone of most pregnancy vaccination schedules.Live vaccines are usually avoided during pregnancy
Live vaccines contain a weakened germ that can reproduce a little in order to create immunity. In pregnancy, they are usually avoided as a precaution, so they are typically planned before pregnancy or after delivery. This is not because they “definitely harm the baby,” but because pregnancy care prefers a wide safety margin when alternatives exist. This type-based rule is one of the main ways modern care differs from the pre-programme era, where practices varied and documentation was inconsistent.Vaccination in pregnancy and the vaccines most women hear about
Specific recommendations depend on your medical history, local guidance, and season, but the reasons behind them are stable. They exist because the pre-vaccine outcomes were worse, therefore prevention has high value.Tetanus and related protection in pregnancy vaccines (Td/Tdap where advised)
Newborn tetanus used to be a real cause of newborn deaths because infection could enter through the umbilical stump, and treatment after onset often came too late. Therefore, tetanus-related vaccination became a core part of antenatal care in order to protect the baby from the first day of life. In some settings, protection against pertussis (whooping cough) is also included (Tdap), because newborn whooping cough can be severe before the baby completes early vaccines. So the pregnancy vaccine is used to transfer antibodies before birth.Flu shot pregnancy and why it is offered
Influenza can cause high fever and significant breathing symptoms, and pregnancy changes lung function and immune responses, so the same virus can cause more disruption than expected. Therefore, flu shot pregnancy is mainly about preventing severe influenza in the mother, and secondarily about passing some antibodies to the baby. The practical point in 2026 India is seasonality: if influenza is circulating and you have exposure risk through work, commuting, or school-going children at home, the preventive value rises.COVID-19 vaccination where currently advised
COVID risk changes with time and local waves, but the decision logic stays the same: severe respiratory illness is harder to manage in pregnancy, so prevention can be safer than infection. Therefore, when current guidance recommends COVID vaccination in pregnancy for your situation, it is usually because expected benefit outweighs expected risk.Hepatitis B and other vaccines in selected situations
Some vaccines are offered based on exposure risk or missing prior protection. This exists because, before organised vaccination, people discovered risk after infection, so modern care tries to prevent predictable infections instead of reacting late.Vaccination in pregnancy and timing that makes sense
Timing is not a superstition. It is cause and effect. If the goal is to protect the mother immediately, vaccination is timed to reduce the “unprotected window,” because waiting leaves a gap where infection can strike. If the goal is to protect the newborn after birth, vaccination is often timed later because antibody transfer to the baby increases as pregnancy progresses, therefore later doses can create stronger newborn protection. So a useful clinic question is: “Is this vaccine mainly for me during pregnancy, or mainly for my baby after birth?” The answer explains timing better than internet schedules.How to decide what is safe for mother and baby in 2026 India
Because WhatsApp forwards are confident and context-free, you need a short method that works under noise.Check the infection risk you are preventing
Ask what infection the vaccine prevents and why it matters in pregnancy or early newborn life. This matters because, in the pre-vaccine era, harm came from underestimating “simple fever.” Therefore, modern care prioritises vaccines that prevent high-impact infections.Check the vaccine type
Confirm whether it is an inactivated vaccine (commonly used) or a live vaccine (usually avoided). This single distinction prevents many errors created by mixed online advice.Check the system: storage and documentation
Vaccines are temperature-sensitive, so the centre should record what you received and when. Keep a photo or digital copy of the record because, in 2026, pregnancy care often spans multiple clinics and labs. Therefore, documentation prevents missed doses, duplicate doses, and confusion at delivery. This is the 1974 lesson in daily life: systems reduce preventable mistakes.Expected side effects and warning signs
Before vaccines, the bigger worry was uncontrolled infection. After vaccines, the bigger worry often becomes normal short-term reactions. The right comparison is mild expected effects versus the risk of severe infection.Common short-term effects
- soreness at the injection site,
- mild fever,
- tiredness or body ache.
Warning signs that need medical advice
Seek care if you have breathing difficulty, facial swelling, widespread hives soon after vaccination, or high fever that persists. Also report reduced fetal movements later in pregnancy, because that needs assessment regardless of vaccination.What commonly goes wrong and how to avoid it
Many failures in the pre-vaccine era were caused by late action. In 2026, failures often come from wrong action.- Skipping a recommended vaccine because of a forwarded story, so the mother faces a preventable infection with high fever, and therefore the pregnancy becomes harder to manage than it needed to be.
- Taking vaccines without a clear record, so follow-up becomes guesswork and errors multiply across visits.
- Delaying a late-pregnancy vaccine until after delivery, so the newborn loses the antibody protection that was the purpose of maternal immunization.
- Buying “add-on” vaccines without a reason, because more injections do not automatically mean more safety.
When to speak to a doctor before vaccination in pregnancy
Discuss timing before vaccination if you currently have a moderate-to-severe illness with fever, a history of severe allergy to a vaccine component, or medical conditions/medicines that suppress immunity. This does not mean refusal. It means planning the safest timing and setting in order to keep risk predictable.Conclusion
Vaccination in pregnancy became important because the pre-vaccine reality was predictable and harsh: infections could become severe in pregnant mothers, and newborns had a dangerous early-life gap before their own vaccines could protect them. The 1974 immunisation programme milestone matters because it turned vaccination into a reliable system—correct selection, cold-chain safety, documentation, and timing—so prevention could replace luck. If you use pregnancy vaccines with clear purpose and clinician-guided timing, maternal immunization can protect both mother and baby in a practical, measurable way. For antenatal vaccination planning with a clear schedule and follow-up, consider BirthRight by Rainbow Hospitals.FAQs
- If pregnancy vaccines did not exist, what would change for my baby? The baby would start life without borrowed antibodies, so the first weeks would depend more on exposure control and chance, and serious infections would be harder to prevent until the baby’s own vaccines take effect.
- Are all pregnancy vaccines safe? No, but the rule is simple: inactivated vaccines are commonly used in pregnancy, while live vaccines are usually avoided. Therefore, safety depends on vaccine type and your clinical context.
- Why is the flu shot pregnancy option discussed so much? Because influenza can cause high fever and breathing symptoms, and pregnancy can increase the chance of severe illness. Therefore, preventing flu is often safer than managing severe flu during pregnancy.
- What should I do if my family WhatsApp group says vaccines cause miscarriage? Treat it as a claim without context. Ask your clinician which vaccine is being discussed, whether it is inactivated or live, and what risk it prevents. So you replace fear with a reasoned decision.
- What if I missed a recommended pregnancy vaccine? Do not self-correct using internet week charts. Ask your clinician what benefit remains at your current stage and what should be planned after delivery, in order to keep the plan purposeful rather than rushed.