Categories
Signs of Down Syndrome During Pregnancy: What You Can Know, Stage by Stage
Sep 19, 2025
There are no reliable “symptoms” a mother feels for Down syndrome. In pregnancy we look for markers on tests, not symptoms. Earliest confirmation is during IVF with embryo testing and later prenatal confirmation. In natural conception, first answers come at 10 weeks with a blood test (NIPT), plus an 11–13 week ultrasound. Only chorionic villus sampling (CVS) or amniocentesis can be diagnosed. Use screening to estimate risk, then decide on a diagnostic test that fits your preferences.
What’s next: Below are the stages - pre-pregnancy, embryo, first and second trimester, and after birth - so you can choose the right test at the right time.
Most cases happen by chance (extra chromosome 21 at conception). A smaller group comes from a translocation that can be inherited. A genetic counselor can review past reports and advise parental karyotyping.
Labs test a few cells from the embryo to look for an extra chromosome 21 (aneuploidy testing). This reduces the chance of transferring an affected embryo but is not considered the final word; most clinicians still advise CVS or amniocentesis later to confirm the pregnancy’s chromosomes.
Useful when: there is a known translocation, repeated pregnancy losses, or advanced maternal age.
NIPT (from 10 weeks): A blood test on the mother that reads tiny fragments of placental DNA. It is very accurate for Down syndrome as a screening test, but it does not diagnose. A high-risk NIPT result should be confirmed with CVS or amniocentesis.
Combined Screening (11-13+6 weeks): Ultrasound nuchal translucency, nasal bone, and a blood test (PAPP-A, free β-hCG). These give a risk number, not a diagnosis.
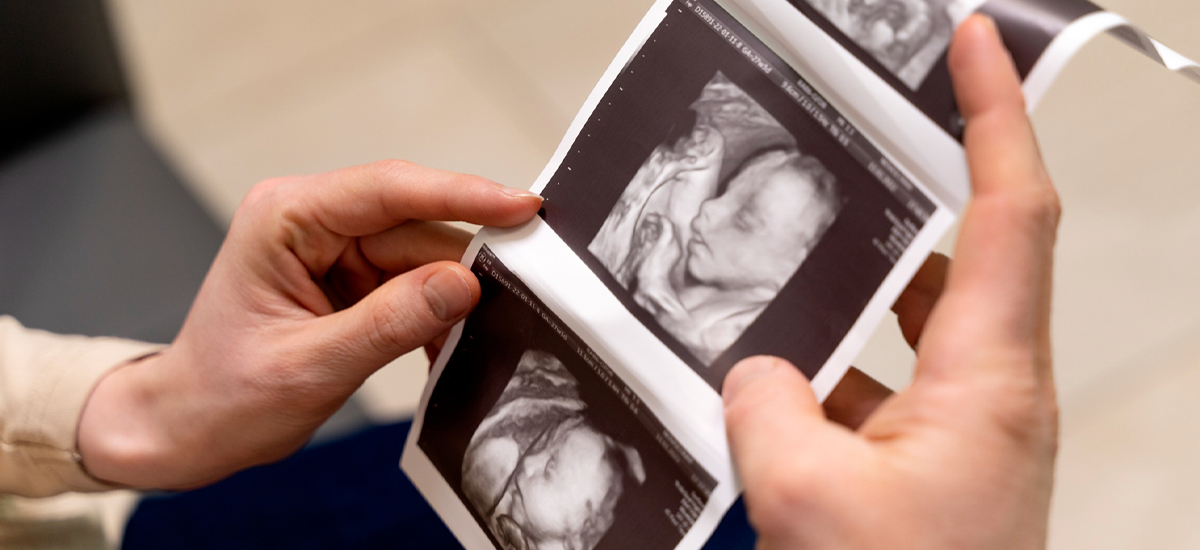
What Ultrasound May Show at This Stage: Increased nuchal translucency or absent nasal bone are markers, not proof. One marker with low-risk bloods is handled differently than several markers together.
Examples: thickened nuchal fold, shorter humerus or femur, absent nasal bone, echogenic intracardiac focus, echogenic bowel, or mild pyelectasis.
Stage 0: Before Pregnancy - Family History And Your Baseline Risk
If Down syndrome runs in the family, start with clear facts.Most cases happen by chance (extra chromosome 21 at conception). A smaller group comes from a translocation that can be inherited. A genetic counselor can review past reports and advise parental karyotyping.
- If a translocation is present in a parent, the recurrence risk is higher and targeted testing is offered in the next pregnancy.
- If not, your risk mainly follows maternal age and general population rates.
Stage 1: Embryo stage (IVF) - What The Lab Can Know
For couples using IVF, embryos can be checked before transfer.Labs test a few cells from the embryo to look for an extra chromosome 21 (aneuploidy testing). This reduces the chance of transferring an affected embryo but is not considered the final word; most clinicians still advise CVS or amniocentesis later to confirm the pregnancy’s chromosomes.
Useful when: there is a known translocation, repeated pregnancy losses, or advanced maternal age.
Stage 2: Weeks 10-13 - First Answers From Blood And Early Ultrasound
This is the earliest window for most natural pregnancies.NIPT (from 10 weeks): A blood test on the mother that reads tiny fragments of placental DNA. It is very accurate for Down syndrome as a screening test, but it does not diagnose. A high-risk NIPT result should be confirmed with CVS or amniocentesis.
Combined Screening (11-13+6 weeks): Ultrasound nuchal translucency, nasal bone, and a blood test (PAPP-A, free β-hCG). These give a risk number, not a diagnosis.
What Ultrasound May Show at This Stage: Increased nuchal translucency or absent nasal bone are markers, not proof. One marker with low-risk bloods is handled differently than several markers together.
| Stage | Test | Window (When) | Clinical Insight (Tells You) | Diagnostic? |
| Early Pregnancy | NIPT | ≥10 weeks | High or low screening risk for Trisomy 21 | No |
| Early Pregnancy | Combined Screen | 11–13+6 weeks | Risk estimate using ultrasound scan + blood markers | No |
| Early Diagnosis | CVS | 11–13+6 weeks | Detailed analysis of fetal chromosomes (karyotype/microarray) | Yes |
Stage 3: Confirmation Options - Cvs Versus Amniocentesis
Choose a diagnostic test if a screen is high risk, if ultrasoundshows multiple markers, or if you want certainty.- CVS (11–13+6 weeks): samples placental tissue through the abdomen or cervix. Gives a definitive chromosome result in the first trimester.
- Amniocentesis (15–20 weeks): samples amniotic fluid. Also definitive.
Both are done by specialists under ultrasound guidance. Your team will explain result times, small procedure risks, and what each test can add (for example, microarray if advised).
Stage 4: Weeks 18–22 - Anatomy Scan And Second-Trimester Clues
The detailed anatomy scan may show “soft markers” that can raise or lower suspicion.Examples: thickened nuchal fold, shorter humerus or femur, absent nasal bone, echogenic intracardiac focus, echogenic bowel, or mild pyelectasis.
- One isolated soft marker with low-risk earlier screening usually does not mean Down syndrome.
- Several markers or a major structural finding prompts review of earlier results and a discussion about amniocentesis if not already done.
| Stage | Test | Window (When) | Clinical Insight (Tells You) | Diagnostic? |
| Mid-pregnancy | Anatomy Scan | 18–22 weeks | Detection of structural findings and "soft markers" | No |
| Mid-pregnancy | Amniocentesis | 15–20 weeks | Definitive analysis of fetal chromosomes | Yes |